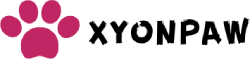Leptospirosis is an infectious and zoonotic disease found throughout the United States. It is caused by a spirochete found in humid environments after being excreted in the urine of reservoir hosts such as raccoons and rats. Because it can affect dogs of any age, breed, and size, and clinical signs can be vague, it is likely underdiagnosed in veterinary patients. “If you don’t test for it, you won’t see it,” said Jessica Pritchard, VMD, MS, DACVIM, clinical assistant professor at the University of Wisconsin School of Veterinary Medicine.
PintoArt / stock.adobe.com

Due to its zoonotic potential, veterinarians must remain vigilant against the disease to protect our staff, clients and other patients. Establishing the diagnosis can be difficult and understanding which patients to test and which tests to use is essential to accurately diagnose the disease. In a session at the Fetch Coastal 2023 conference, Pritchard discussed current recommendations for the diagnosis, treatment and prevention of leptospirosis.1
Clinical presentation
“What many of us learned in veterinary school is that leptospirosis is a jaundiced dog with kidney failure,” Pritchard said. “But it can also be azotemia without liver damage, liver damage without azoles, both, or, frustratingly, neither.” In a study of 51 dogs definitively diagnosed with leptospirosis, 75% had azotemia, 14% had liver damage alone, and 1 dog had lung damage.2 The most common clinical signs included anorexia, vomiting, lethargy, and polyuria and polydipsia (PU/PD).2 Lung involvement appears to be more common in Europe.
There are no pathognomonic clinical signs or biological changes. What is observed in the patient and in the laboratory will depend on the organs affected by the leptospires. Dogs are exposed when the organism passes through their mucous membranes from the environment. After infection, leptospires travel through the bloodstream to their organ of choice. Laboratory changes may include any combination of azotemia, elevated alanine transaminase (ALT), alkaline phosphatase. (ALP) and total bilirubin.
“Because of all the different places lepto goes (in the body), diagnosis can be difficult,” advised Pritchard, emphasizing the importance of the timeline of the infection:
- Day 0: Mucosal penetration of infectious organisms
- Day 4: Significant leptospiremia is present due to replication of the organism. IgM is measurable.
- Days 5 to 7: Vascular damage and thrombocytopenia may be observed.
- Date 7: Clinical signs are noticeable.
- Day 10: Leptospiremia disappears and IgG levels increase.
- Day 15: Renal colonization has occurred (if it is expected to occur) and urinary excretion begins.
Diagnostic tests
Understanding the timeline of the infection allows veterinarians to choose the tests most likely to give them a definitive diagnosis. Often, multiple tests are necessary. The tests look for the organism directly or detect exposure by the presence of antibodies.
Direct detection of the organism is done by polymerase chain reaction (PCR), which searches for leptospirosis DNA. A positive PCR test demonstrates active infection and is not influenced by previous illness or vaccination. However, a negative test does not rule out infection. Pritchard uses a fishing analogy to explain this to clients: Just because you don’t catch fish (or get a positive PCR) doesn’t mean there aren’t any fish (or leptospires) at all, this means that there are none. none in the small area you checked.
PCR can be performed on urine, blood, or both. The best sample to submit will depend on where you think you are in the disease timeline and where you think the organisms are most likely to be found. Samples should be collected before starting antibiotic treatment, as even a short course of antibiotics can create a false negative.
Indirect tests look for antibodies in the submitted sample. The microscopic agglutination test (MAT) is most commonly used. One of the advantages of this test is that it can identify the serovar causing the infection. Because this test must be sent to a specific laboratory for testing, results will be delayed. Additionally, the test can be positive for 3 reasons: current infection, previous vaccination or previous exposure.
Point-of-care antibody testing is available to provide faster results. The IDEXX SNAP Lepto test screens for antibodies against the most abundant outer membrane protein in pathogenic strains (LipL32). Although it provides rapid results, it may be affected by vaccination status. The Zoetis Witness IgM test is also available as a point-of-care test. It appears to have high sensitivity and specificity, is less likely to be affected by vaccination and IgM testing, which can be detected on day 4 of infection, potentially providing earlier diagnosis.
Pritchard’s recommendation is to collect samples for PCR and acute MAT if leptospirosis is suspected, then begin antibiotic treatment. If the PCR test is positive, the diagnosis is clear. If the PCR test is negative, a convalescent MAT will be required to demonstrate at least a fold increase in antibody levels and confirm infection. Pritchard encourages veterinarians to confirm the diagnosis with matched titers because of the zoonotic potential. One recommendation is to charge for paired titles in advance to encourage customers to bring their pets back for the second sample.
Treatment, prognosis and prevention
“Treatment for leptospirosis, unlike diagnosis, is actually quite simple,” Pritchard said. In the early stages of the disease, potentiated penicillins are used to eliminate leptospiremia. Doxycycline at 5 mg/kg BID for 14 days is necessary to cleanse the tissues. Overall, a survival rate for the disease is 80%, although some patients require dialysis to survive, which is not an option for all clients, due to location and /or cost. People with lung damage often have a poorer prognosis.
Pritchard shared that “what’s frustrating to me about leptospirosis and how it occurs so frequently is that it is a vaccine-preventable disease.” Although leptospirosis is classified as a lifestyle vaccine in the American Animal Hospital Association vaccination guidelines,3 Recent studies have shown that all dogs can be at risk, including small breed dogs.4 Although many clients are concerned about the safety of the leptospirosis vaccine, adverse effects are rare.5
Takeaways
Leptospirosis is found throughout the United States and is probably more common than previously thought. Accurate diagnosis is essential for both patient treatment and protection of humans from zoonotic diseases. Obtaining an accurate diagnosis often requires multiple tests, and the best choice of test will vary depending on how long the patient has been infected. Once the samples are collected, treatment can be started. All dogs should be considered candidates for the leptospirosis vaccine, as the disease is prevalent but highly preventable through vaccination.
The references
- Prtichard J. Leptospirosis updates: current concerns and protecting our patients. Presented at the Fetch dvm360 conference; Atlantic City, New Jersey. October 9-11, 2023.
- Tangeman LE, Littman MP. Clinicopathological and atypical characteristics of natural leptospirosis in dogs: 51 cases (2000-2010). J Am Vet Med Assoc. 2013;243(9):1316-22.
- Ellis J, Marziani E, Aziz C et al. AAHA Canine Vaccination Guidelines 2022. J Amer Anim Hosp Assoc. 2022; 58:1-19. doi: 10.5326/JAAHA-MS-Canine-Vaccination-Guidelines
- Lee HS, Guptill L, Johnson AJ and Moore GE. Reporting changes in canine leptospirosis between 1970 and 2009. J Vet Intern Med. 2014;28(2):294‐9.doi: 10.1111/jvim.12273
- Moore GE, Morrison J, Saito EK et al. Breed, lower weight, and multiple injections are associated with increased reports of adverse events within three days of canine vaccine administration. J Am Vet Med Assoc. 2023;14:1-7. doi: 10.2460/javma.23.03.0181